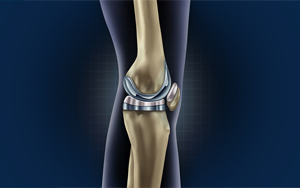
Total Knee Replacement
Knee replacement surgery or knee arthroplasty where our knee joint is replaced with man-made artificial joint...
Enter your contact details here to help us serve you better & faster.

In addition to our excellent joint replacement services, conditions treated by Dr. Amit Nath Misra are:
All kinds of orthopaedic treatment under one roof with us.
SKI Clinic is renowned for its highly experienced & skilled joint replacement surgeon treating innumerable orthopaedic cases.